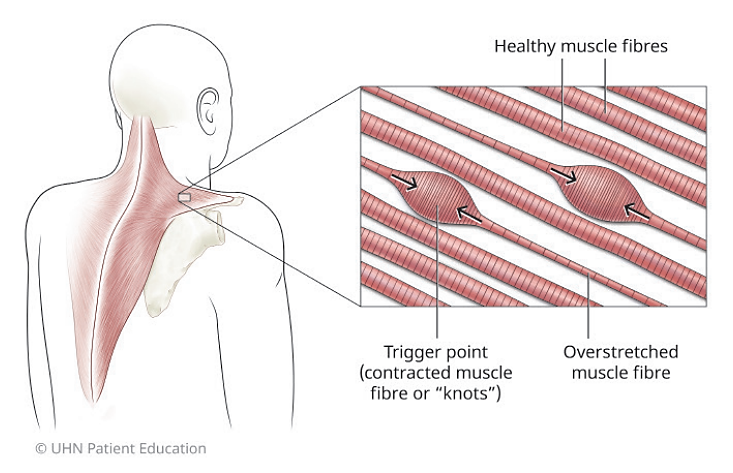
Myofascial Pain Syndrome is a chronic pain disorder caused by overactive trigger points in a distinct section of the body. Anatomically, trigger points are created by muscle fibers that get stuck in a contracted state and can’t fully return to resting length after muscle contraction. These shortened muscle fibers result in overlapped muscle tissue and create a dense area of muscle, commonly referred to as a “knot.” These knots can be identified using palpation due to the increased density of muscle tissue and the heightened local sensitivity to touch.
Overactive trigger points turn into Myofascial Pain Syndrome when they begin to create a pain response in the body. With chronic contraction of muscle fibers, blood flow and oxygen input to muscle tissue diminishes. This allows cellular waste to build up inside of the muscle, which produces pain in that local area. As the cellular waste builds up and the pain signal intensifies, it causes further muscle tightness, muscle weakness, and sometimes even loss of joint mobility.
Causes, Symptoms, and Related Health Concerns
Myofascial Pain Syndrome can be caused by injury, repetitive motions, poor posture, stress-related muscle tension, and external pressure. Other times, these sensitive points in your muscles have no obvious cause. When trigger points don’t resolve and when your pain persists over time despite intervention, it is diagnosed as Myofascial Pain Syndrome. Signs and symptoms of Myofascial Pain Syndrome can include:
- A sensitive knot in a muscle, especially with unknown cause
- Deep, aching, or throbbing muscle pain which can occur even at rest
- Muscle pain that doesn’t resolve or that worsens over time
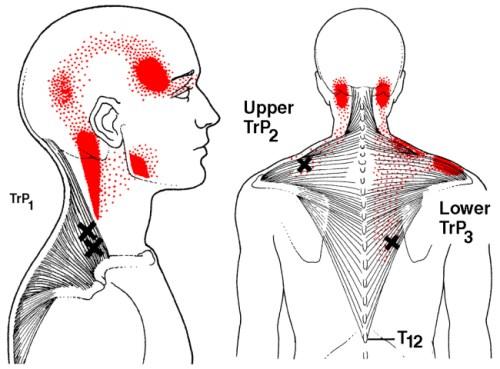
Those most at risk of Myofascial Pain Syndrome are middle-aged, inactive women. The parts of the body that are most often affected are the neck, upper back, and shoulders. However, Myofascial Pain Syndrome can occur in any muscle and can result in local or referred pain. Local pain is easier to identify, while referred pain can require a more skilled eye. There are various charts describing referred pain patterns, with Travell, Simons, & Simons being the most well documented resource. Below is an example of a referred pain pattern for the upper trapezius muscle.
Coinciding health problems can include fatigue, poor sleep, stress, and headaches. If you are experiencing muscle pain throughout the entire body, this is more likely to be Fibromyalgia, as Myofascial Pain Syndrome is local to one area of the body. Fibromyalgia is often associated with greater symptom intensity, including an increased number of trigger points, greater fatigue and sleep disturbance, and more severe headaches due to the brain becoming hypersensitive to pain and requiring a lower threshold to stimulate a pain response.
Diagnosis and Treatment
There are no imaging or laboratory tests that diagnose Myofascial Pain Syndrome. The best method for diagnosis is a physical examination, including palpation of trigger points or “knots”, as well as assessment of muscle strength, flexibility, range of motion, and posture.
Treatment can vary depending on the extent of your symptoms.
- Home treatment strategies include heat, over-the-counter pain medications (such as non-steroidal anti-inflammatory drugs or NSAIDs), and relaxation techniques. Evidence also supports that participating in low-impact exercise and correcting poor postural habits provide relief from symptoms of Myofascial Pain Syndrome.
- Physical therapy treatments include soft tissue massage and trigger point dry needling, therapeutic exercise, and use of modalities (such as ultrasound and transcutaneous electrical nerve stimulation).
- Physician treatments include prescribing medications and administering trigger point injections.
If you are experiencing muscle pain that does not go away, make an appointment with one of our physical therapists to be evaluated for Myofascial Pain Syndrome and get back to the pain-free lifestyle you once had!